-
Author
Anwesha Dubey -
PI
Aria Fallah and Anthony Wang
-
Co-Author
Andrew Wang, Keshav Goel, Alexander G. Weil, Aria Fallah
-
Title
Operative Outcomes Following Hemispherectomy versus Hemispherotomy for the Treatment of Hemimegalencephaly in Pediatric Patients: A Systematic Review
-
Program
STTP
-
Other Program (if not listed above)
-
Abstract
Operative Outcomes Following Hemispherectomy versus Hemispherotomy for the Treatment of Hemimegalencephaly in Pediatric Patients: A Systematic Review
Anwesha Dubey, BS[1], Andrew Wang, MAS[1], Keshav Goel, BS[1], Alexander G. Weil, MD[2], Aria Fallah, MD, MS[1,3]
[1]David Geffen School of Medicine at UCLA, Los Angeles, CA, United States
[2]Division of Neurosurgery, University of Montreal, Montreal, Quebec, Canada
[3]Department of Neurosurgery, UCLA Mattel Children’s Hospital, Los Angeles, CA, United States
Introduction: Hemimegalencephaly (HME) presents with a triad of classic clinical features: epilepsy, contralateral motor deficits, and neurocognitive issues. In most cases, epilepsy is the first manifestation of HME with many patients progressing to drug-resistant seizures that are best treated by hemispherectomy or hemispherotomy. Due to the infrequency of HME in the general population and the heterogeneity of disease presentation, there exists a paucity of literature with inconsistent conclusions on the outcomes of these surgeries.
Objectives: This study hopes to determine the efficacy of hemispherectomy vs. hemispherotomy in improving seizures and assess relevant postoperative outcomes of HME patients over a long-term follow-up period. Additionally, we will correlate preoperative data with postoperative seizure status to identify the factors that render a favorable prognosis after surgical treatment.
Methods: A comprehensive literature search (PubMed, Embase, and Scopus) was conducted with no restrictions in regard to language, date, or country of origin to identify articles that reported outcomes of HME pediatric patients undergoing hemispherectomy or hemispherotomy. Two independent reviewers then assessed the eligibility of studies based on inclusion and exclusion criteria. For each study, the authors recorded the rates of seizure freedom (i.e. Engel class), improvement in motor and neurocognitive impairment, and plausible preoperative factors that could be associated with seizure outcomes. Univariate Cox regression was conducted to evaluate the efficacy of the two surgical procedures and identify which of the preoperative variables were associated with seizure freedom. A Kaplan-Meier plot was also created.
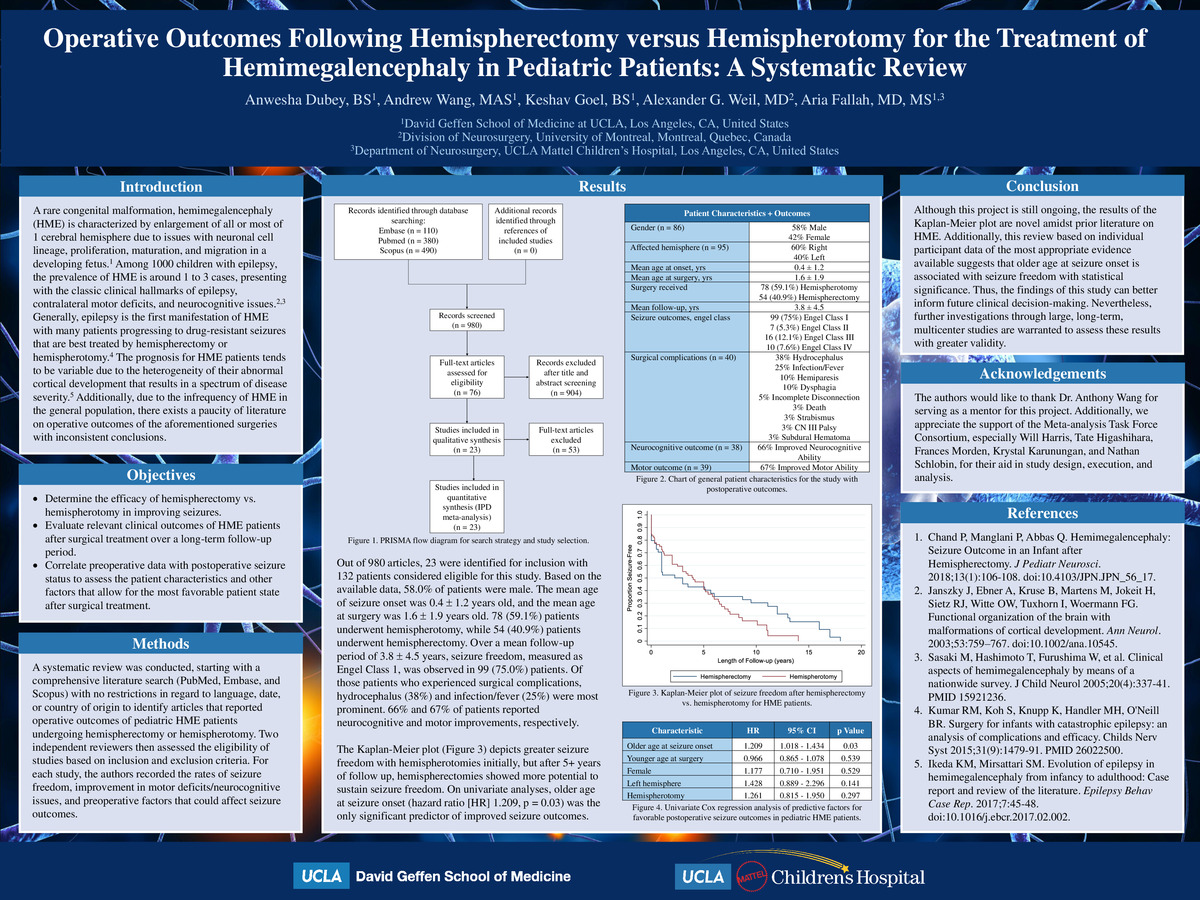
Results: After a review of 980 citations, 23 articles reporting on 132 patients were eligible for this study. Of the included participants, the mean age of seizure onset was 0.4 ± 1.2 years old, and the mean age at surgery was 1.6 ± 1.9 years old. 78 (59.1%) patients underwent hemispherotomy, while 54 (40.9%) patients underwent hemispherectomy. Over a mean follow-up period of 3.8 ± 4.5 years, seizure freedom (Engel Class 1) was observed in 99 (75.0%) patients. On univariate analyses, older age at disease onset (hazard ratio [HR] 1.209, p = 0.03) was the only statistically significant predictor of improved seizure outcomes. The Kaplan-Meier plot depicted greater seizure freedom with hemispherotomies initially, but after 5+ years of follow up, hemispherectomies showed more potential to sustain seizure freedom.
Conclusion: Although this project is still ongoing, the results of the Kaplan-Meier plot are novel amidst prior literature on HME. Additionally, this review based on individual participant data of the most appropriate evidence available suggests that older age at seizure onset is associated with seizure freedom with statistical significance. These findings can inform future decision making; however, further investigations through large, long-term, multicenter studies are warranted to assess these results with greater validity.
-
PDF
-
Zoom
https://uclahs.zoom.us/j/91290198569?pwd=S1BJaEJkZnhIeVBtMW8rZzVXVGI3QT09