-
Author
Joy Ohiomoba -
PI
Christopher Tarnay, MD
-
Co-Author
Martha Mbenia Musyoka, MD
-
Title
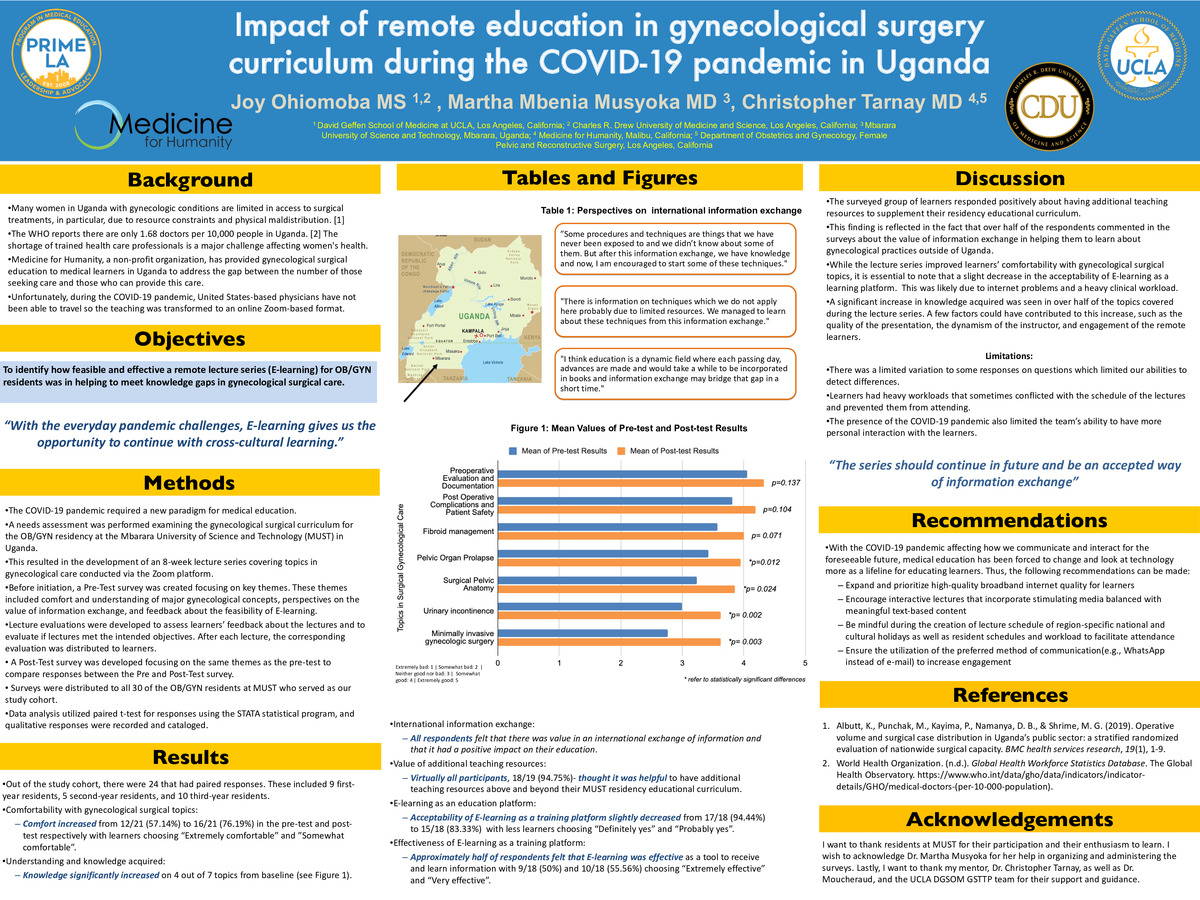
Impact of remote education in gynecological surgery curriculum during the COVID-19 pandemic in Uganda
-
Program
Global Short-Term Training Program
-
Other Program (if not listed above)
-
Abstract
Background:
Many women in Uganda with gynecologic conditions are limited in access to surgical treatments due to resource constraints and physical maldistribution. A shortage of trained healthcare professionals remains a leading cause, and there is a need to ensure that there are trained medical professionals to care for women’s health issues. Medicine for Humanity, a nonprofit organization, has provided gynecological surgical education to medical learners in Uganda to address the gap between the number of those seeking care and those who can provide this care. Unfortunately, during the COVID-19 pandemic, United States-based physicians have not been able to travel. Thus, the teaching focusing on topics in gynecological care has transformed to being an online format.
Methods:
An 8-week lecture series covering topics in gynecological care was developed and conducted via the Zoom platform for the OB/GYN residency at the Mbarara University of Science and Technology (MUST) in Uganda. Before initiation, a Pre-Test survey was created focusing on key themes such as understanding of major concepts, perspectives on information exchange, and feedback about the feasibility of E-learning. Lecture evaluations were developed to assess lecture feedback and to evaluate if lectures met the intended objectives. After each lecture, the corresponding lecture evaluation was distributed to learners. A Post-Test survey was also developed with the same themes as the pre-test survey. For data analysis, we did a paired t-test using the STATA platform and examined the content of the qualitative responses.
Results:
There were a total of 30 residents that were sent surveys with 24 residents that had paired responses. The results showed that comfort in surgical gynecological topics increased from 12/21 (57.14%) to 16/21 (76.19%) in the pre-test and post-test, respectively, with learners choosing “Extremely comfortable” and ”Somewhat comfortable.” The learners’ understanding and knowledge acquired significantly increased on 4 out of 7 topics, and almost all participants thought it was helpful to have additional teaching resources above and beyond their MUST residency educational curriculum. Acceptability of E-learning as a learning platform slightly decreased from 17/18 (94.44%) to 15/18 (83.33%), and about half of the respondents felt that E-learning was effective as a platform to receive and learn information.
Discussion and Conclusion:
The learners responded positively about having teaching resources supplementing their residency educational curriculum, with several providing comments about their perspectives on information exchange. Additionally, the lecture series improved learners’ comfort with gynecological topics. Still, there was a slight decrease in learners who felt that E-learning was an acceptable learning platform. This was likely due to issues such as internet problems and workload conflicts. Lastly, the statistically significant differences seen in over half of the topics covered showed that knowledge gaps in surgical gynecological care were being filled. With the COVID-19 pandemic affecting the way we interact for the foreseeable future, medical education has been forced to change and look at technology, like our Zoom-based lecture series, as a lifeline for educating students and advancing learning.
-
PDF
-
Zoom
https://uclahs.zoom.us/j/96090813269?pwd=SDZEQWxVaVpjenZSOVhUNlNGVkJTZz09