-
Author
Vishnu Murthy -
PI
Andrei Gafita, MD
-
Co-Author
Johannes Czernin, Michael Hofman, Wolfgang Fendler, Louise Emmett, Clemens Kratochwil, Matthias Eiber, Ida Sonni, Matthias Benz, Thomas Hope, Andrea Farolfi, Irene Burger, Jérémie Calais, Masatoshi Hotta
-
Title
Predicting Outcomes of Metastatic Castrate-Resistant Prostate Cancer Patients after Lutetium-177 PSMA Radioligand Therapy
-
Program
STTP
-
Other Program (if not listed above)
-
Abstract
Objective:
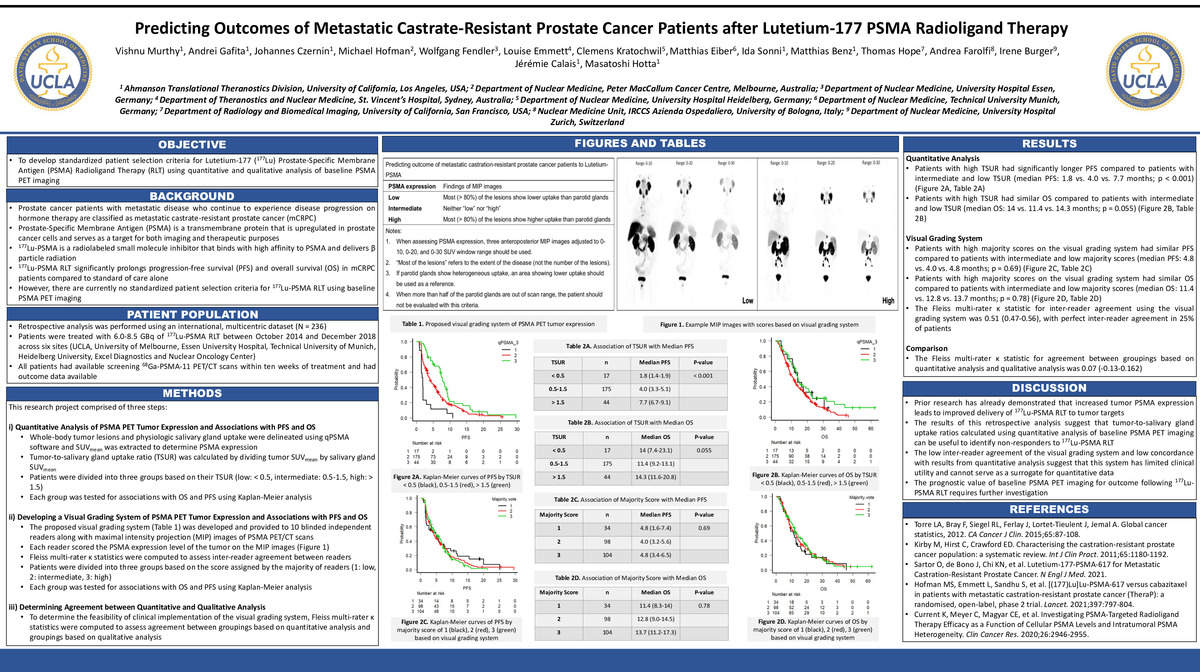
To develop standardized patient selection criteria for Lutetium-177 (177Lu) Prostate-Specific Membrane Antigen (PSMA) Radioligand Therapy (RLT) using quantitative and qualitative analysis of baseline PSMA PET imaging.
Introduction:
Prostate cancer patients with metastatic disease who continue to experience disease progression on hormone therapy are classified as metastatic castrate-resistant prostate cancer (mCRPC). 177Lu-PSMA RLT significantly prolongs progression-free survival (PFS) and overall survival (OS) in mCRPC patients compared to standard of care alone. However, there are currently no standardized patient selection criteria for 177Lu-PSMA RLT using baseline PSMA PET imaging.
Methods:
Retrospective analysis was performed using an international, multicentric dataset (N = 236). Patients were treated with 6.0-8.5 GBq of 177Lu-PSMA RLT between October 2014 and December 2018 across six sites and had available screening 68Ga-PSMA-11 PET/CT scans within ten weeks of treatment. This research project comprised of three steps: i) quantitative analysis of PSMA PET tumor expression and determination of associations with OS and PFS ii) development of a visual grading system of PSMA PET tumor expression and determination of inter-reader agreement and associations with OS and PFS and iii) determining agreement between quantitative and qualitative analysis.
Results:
Patients with high tumor-to-salivary gland uptake ratios on baseline PSMA PET imaging had significantly longer PFS compared to patients with intermediate and low tumor-to-salivary gland uptake ratios (median PFS: 1.8 vs. 4.0 vs. 7.7 months; p < 0.001) but similar OS (median OS: 14 vs. 11.4 vs. 14.3 months; p = 0.055). Patients with high majority scores on the visual grading system had similar PFS compared to patients with intermediate and low majority scores (median PFS: 4.8 vs. 4.0 vs. 4.8 months; p = 0.69) and similar OS (median OS: 11.4 vs. 12.8 vs. 13.7 months; p = 0.78). The Fleiss multi-rater κ statistic for inter-reader agreement using the visual grading system was 0.51 (0.47-0.56), while the Fleiss multi-rater κ statistic for agreement between groupings based on quantitative analysis and qualitative analysis was 0.07 (-0.13-0.162).
Conclusions:
Tumor-to-salivary gland uptake ratios calculated using quantitative analysis of baseline PSMA PET imaging can be useful to identify non-responders to 177Lu-PSMA RLT. The low inter-reader agreement of the visual grading system and low concordance with results from quantitative analysis suggest that this system has limited clinical utility and cannot serve as a surrogate for quantitative data. The prognostic value of baseline PSMA PET imaging for outcome following 177Lu-PSMA RLT requires further investigation.
-
PDF
-
Zoom